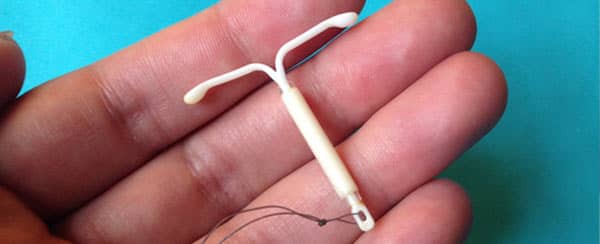
Note: Bayer submitted a Supplemental New Drug Application (sNDA) for Mirena in October 2019. The sNDA seeks to extend Mirena's labeling to allow use up to six years. As of July 2020, the sNDA is still underway. Mirena is currently approved for only five years of use.
Mirena lawsuits claim the birth control device causes serious side effects. The intrauterine device (IUD) has migrated, perforating the uterus in some cases. The IUD has also been linked to increased pressure in the brain. At least 2,700 women have sued Bayer over these adverse events. Some of these cases settled in 2018 for $2.2 million.
Why Women Are Filing Mirena Lawsuits
Mirena lawsuits stem from the device's severe side effects. In early 2018, Bayer announced a settlement that resolved thousands of Mirena-related lawsuits. The settlement only included claims related to IUD migration and perforation.
However, many women have sued Bayer due to a serious condition known as pseudotumor cerebri ("false tumor"). This condition can cause tumor-like symptoms in the brain. Bayer's 2018 settlement did not settle any cases related to pseudotumor cerebri. These cases are still pending.
- Device migration
- Device embedment
- Organ perforation
- Pseudotumor cerebri
- Ectopic pregnancy
Pseudotumor Cerebri / Idiopathic Intracranial Hypertension
Pseudotumor cerebri (PTC) is a buildup of pressure in the brain. It is also known as idiopathic intracranial hypertension (IIH).
Increased pressure can exert force on the brain, leading to a number of symptoms similar to a brain tumor. These can include vision changes, balance issues, and mental or memory problems.
PTC can happen to anyone, but certain medications can increase the risk. Among those drugs is levonorgestrel. Levonorgestrel is the progestin-based hormone used in Mirena. A 2015 study by Canadian researchers demonstrated this effect. In the study, women who used Mirena were more likely to develop PTC than women who did not use Mirena.
Women who have experienced PTC while using a Mirena IUD could be eligible for compensation.
Symptoms of Pseudotumor Cerebri
- Vision changes (e.g., double vision, loss of vision, etc.)
- Dizziness
- Headaches
- Nausea
- Vomiting
- Depression
- Neck stiffness
- Difficulty walking
- Tinnitus (ringing in the ears)
- Memory problems
Ectopic Pregnancy
An ectopic pregnancy occurs when a fertilized egg attaches to a structure outside the uterus. Most ectopic pregnancies occur in the fallopian tube, the structure connecting the uterus to the ovary.
This type of pregnancy can cause life-threatening complications like bleeding and fallopian tube rupture. More than 1,200 ectopic pregnancies have been reported by Mirena users.
FDA Warnings About Mirena IUD Marketing
In April 2009, the FDA warned Bayer and the public about the company's misleading Mirena marketing. Mirena should only be used for up to five years before replacement. However, Bayer's marketing did not include this information. Instead, the initial marketing implied the IUD could be used indefinitely. Bayer also failed to state that Mirena was primarily recommended for women who already had at least one child.
The FDA's Adverse Events Reporting System (FAERS) keeps track of device injuries. As of July 2020, FAERS includes 104,000 reports concerning Mirena. Motivated by these injuries, thousands of women have filed lawsuits against Bayer. Many of these women make similar legal complaints. Specific allegations claim Bayer:
- Designed, produced, and knowingly sold a defective product
- Failed to research and warn the public about dangerous side effects
- Concealed the dangerous side effects
- Engaged in false and misleading marketing
- Misrepresented the benefits of the device
- Breached implied and express warranty
- Failed to issue a recall once the information came to light about the complications
Mirena Multidistrict and Multicounty Litigation
Bayer has settled thousands of Mirena lawsuits. But, there are still some cases pending. Many individual Mirena lawsuits have been consolidated into federal multidistrict litigation (MDL). Others have been consolidated into multicounty litigation (MCL) in state courts. There are currently three sets of mass torts covering Mirena IUDs:
- MDL 2434 in United States District Court
- MDL 2767 in United States District Court
- NJ MCL 297 in New Jersey State Courts
MDL 2767: Mirena Pseudotumor Cerebri
Many women have experienced complications due to a buildup of pressure in the brain. This is known as pseudotumor cerebri (PTC). This condition has symptoms similar to a brain tumor. Research studies have linked the hormone in the Mirena IUD with this dangerous condition.
In April 2017, the U.S. Judicial Panel on Multidistrict Litigation (JPML) consolidated all Mirena PTC lawsuits. They formed MDL 2767 in the Southern District of New York. This included 113 pending Mirena cases in 17 districts and 37 potential actions. As of July 2020, more than 900 cases had been filed in this MDL.
MDL 2434: Mirena Migration, Perforation and Embedment
In June 2013, the JPML consolidated many Mirena IUD lawsuits into an MDL in the Southern District of New York. These cases claim complications due to:
- Device migration
- Organ perforation
- Device embedment
The MDL argued Mirena's initial label did not contain warnings about secondary perforation. The label in question was used from 2008 through 2014. It did state that Mirena IUD perforation may occur during insertion and escape detection until sometime later. But claimants said the contraceptive device could cause perforation at any time.
The majority of these cases were settled in April 2018.
New Jersey MCL 297
Many plaintiffs in New Jersey made similar allegations to those in the New York MDL. So the NJ Supreme Court consolidated cases in multicounty litigation (MCL) in 2013.
In April 2018, Judge Rachelle Harz appointed a Special Master. The Special Master would oversee settlement negotiations between Bayer and plaintiffs in MCL 297. Garretson Resolution Group was appointed in June 2018 as the lien resolution administrator. This settlement was part of the 4,100-case settlement announced by Bayer in April 2018.
Individual Mirena IUD Lawsuits
The first Mirena IUD lawsuits generally concerned device migration. Below is a summary of complications experienced by some of the earliest claimants:
Desaree Nicole Lee Johnson suffered pain when her Mirena IUD perforated her uterus and moved into her abdomen. After undergoing surgery to remove it, she became pregnant. She then experienced vaginal bleeding and had a miscarriage. She claims Bayer knowingly released an unsafe and defective product. She also says their actions directly lead to her injuries.
Melody Williams began experiencing severe pain and abdominal cramping. It had been less than a year since her Mirena IUD was implanted. As a result, Williams required surgical removal of the device. The first removal failed. Surgeons attempted a second procedure and found the IUD had migrated through her fallopian tube. Williams experienced pain, distress, and numerous medical procedures as a result of the IUD. She and her husband filed a suit accusing Bayer of negligence and reckless disregard for public safety.
Mirena Lawsuit Settlement Amounts
In April 2018, Bayer signed an agreement to settle approximately 4,000 Mirena lawsuits. The settlement related to claims of perforations caused by the IUD. The settlement includes cases in federal MDL 2434 and NJ MCL 297. It also included cases filed in St. Louis City Circuit Court (Missouri) and all pending cases in California.
The total settlement amount was $12.2 million. But, individual settlement amounts for Mirena lawsuits vary depending on the details of each individual case.
This settlement only resolved cases related to perforation by the Mirena device. Other claims related to ectopic pregnancy and idiopathic intracranial hypertension (ITC) are still outstanding.
Mirena Lawsuit FAQs
Can I File a Mirena Lawsuit?
Women who received a Mirena IUD implant and experienced one of the following severe side effects may be eligible for compensation (legal damages):
- Perforation of the uterus or another organ
- Migration of the device
- Intense cranial pressure or headaches - idiopathic intracranial hypertension (ITC) or pseudotumor cerebri (PTC)
- Unintended pregnancies
- Ectopic pregnancies or other pregnancy complications
How Much Is the Mirena Lawsuit Individual Settlement Amount?
The Mirena settlement announced in April 2018 covered about 4,000 perforation cases. The total settlement amount announced in Bayer's financial filings was $12.2 million. This amounts to about $3,050 per person. However, the exact amount will differ based on the final number of plaintiffs who agree to the settlement. Adjustments may also be made based on the severity of each individual's case.
Additional settlements could be reached for other outstanding cases. This may include plaintiffs who choose not to sign onto the April 2018 settlement. If your Mirena IUD caused a serious side effect, you should consider starting legal action. Don't wait, because each state has its own deadline (statute of limitations).
What Does a Mirena Lawyer Cost?
Mirena lawsuits, like other medical device lawsuits, are filed on what is known as a contingency basis. This means that you will not have to pay anything up front. Instead, you will only pay legal fees if you win money for your claim either through a verdict or settlement.